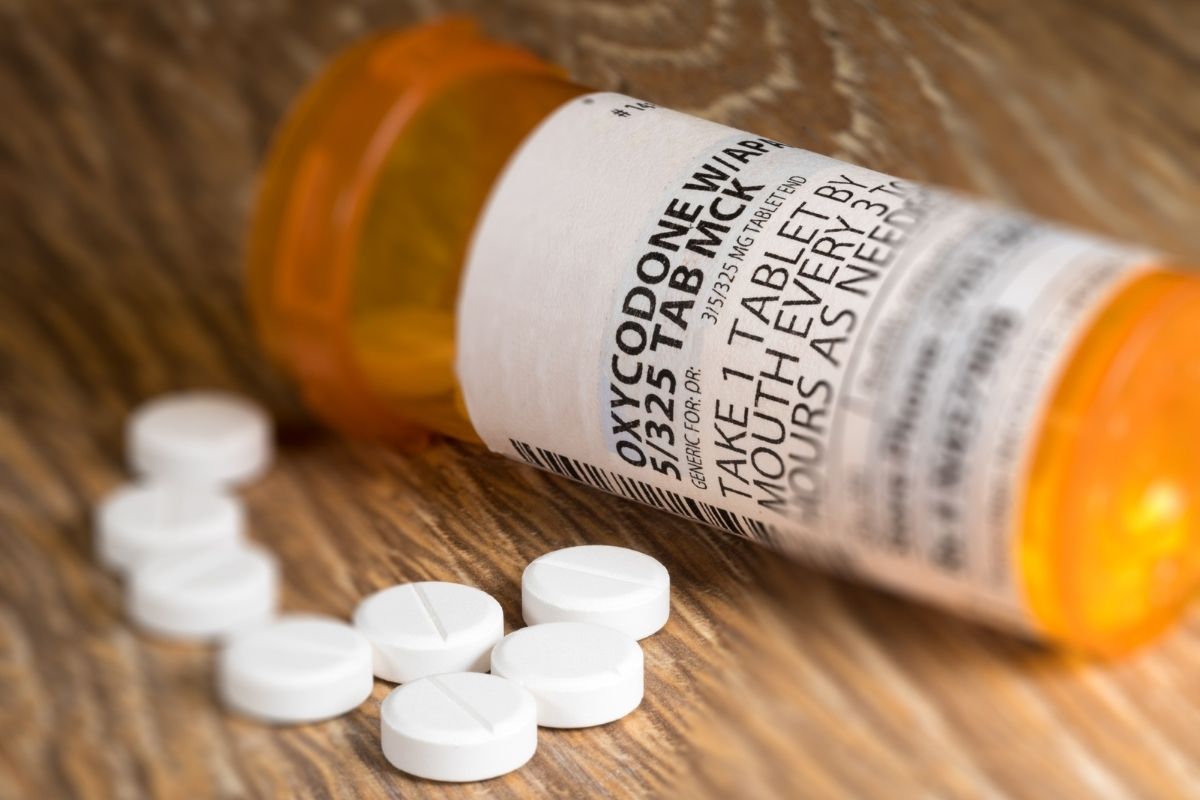
Treatment of drug addiction has become a standard of health care. This is why access to medicines like Suboxone is essential for many who participate in rehabilitation programs.
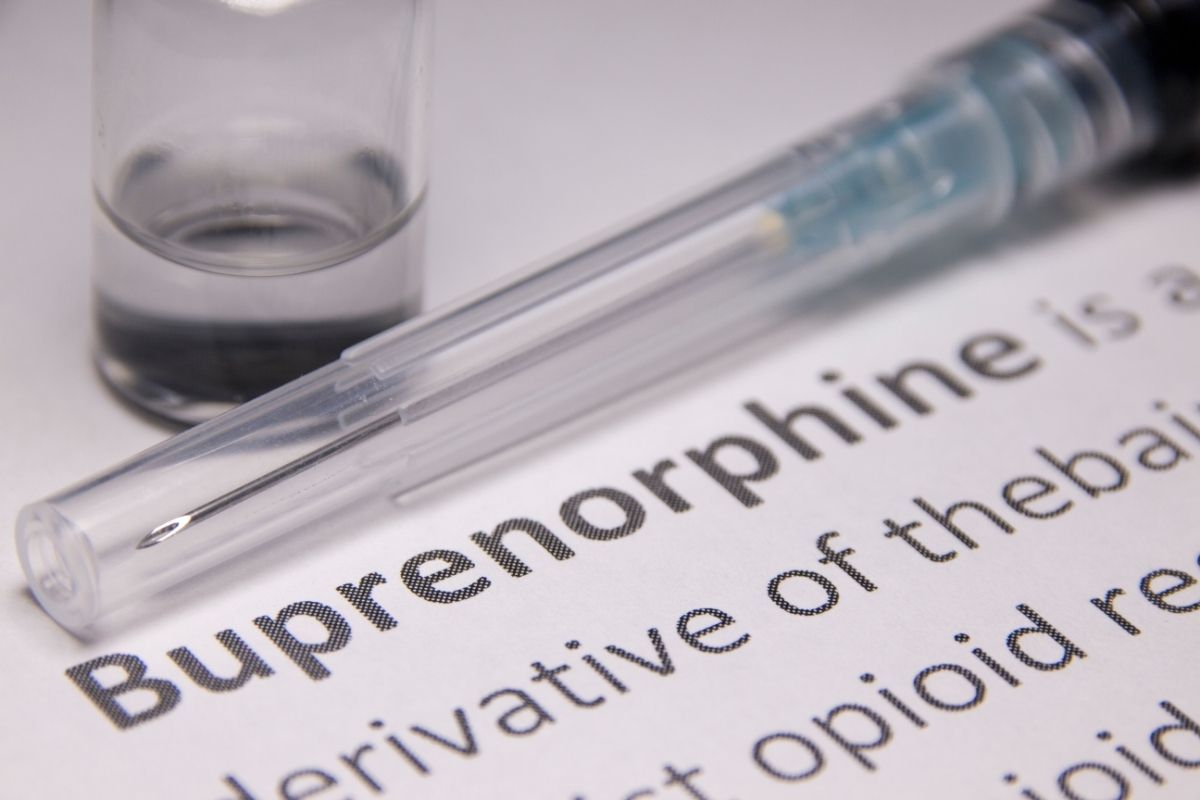
For example, buprenorphine, the main ingredient in Suboxone, is widely used to treat opioid addiction and is an important part of recovery for many.
Inquiring about Saboson quantity limits and other exclusions at Anbetter Health Insurance Company.
Is Suboxone Covered By Ambetter Health Insurance?
Yes, the use of Suboxone is covered by Ambetter Health Insurance under most health care plans and policies.
Because Suboxone is a widely used drug for opioid addiction, insurance companies usually cover the cost.
Health plans that also cover mental health are required by the Mental Health and Addiction Equality Act to provide coverage equivalent to health insurance.
As a result, access to addictive drugs such as Suboxone has improved significantly in recent years. ambetter complaints, ambetter of tennessee doctors list, ambetter telemedicine
called customer service, complaints filed, all the other hospitals
The legislation also facilitated wider access to mental health care, making medicines more readily available to most patients.
However, the exact details of your Anbetter Insurance coverage will depend on the plan you choose and the specific policy.
The best way to find out if the Ambetter plan covers the cost of his Suboxone is to check the policy.
Please read the fine print of the policy and review the exclusions.
Alternatively, you can contact Ambetter to see if your use of Suboxone is covered under current policies.
Do rehab centers accept better insurance?
Whether rehab centers allow insurance for patients’ costs is typically their choice. Not every state where Ambetter provides health care includes a rehabilitation program for alcohol rehabilitation which includes Ambetter coverage.
However, the coverage can cover out-of-state treatment of addictions too. This may mean the possibility of going to your preferred recovery facility if you want proper care. Ambetter provides partial or total coverage for in-home rehabilitation, based on your insurance coverage for certain conditions. dr.that prescribes suboxone, online suboxone doctors that accept medicaid, online subutex doctors that accept medicaid, prescribe suboxone, suboxone doctors, withdrawal symptoms opioid use disorder, opioid addiction treatment methadone clinics, addiction medicine.
suboxone doctors near me, ambetter cms standard gold, cvs ambetter, online subutex doctors that take insurance, pharmacy program benefits, plan benefits print, company language access, member online account view. ambetter reviews, pros and cons of ambetter insurance, ambetter health insurance reviews, ambetter home state health reviews, health, insurance marketplace, health insurance plans, ambetter health insurance review
health insurance companies
What Suboxone Quantity Does Ambetter Cover?
The genuine amount of dependancy medicine, which include Suboxone, included through Ambetter relies upon for your plan, and your particular policy.
Some plans cowl a amount of Suboxone two times daily, at the same time as different plans cowl the charges for 3 instances daily.
This does additionally rely upon your doctor’s prescription and your scientific needs.
Some insurers provide handiest partial insurance of medicine, at the same time as others cowl the total charges of Suboxone remedy.
Ambetter, which gives healthcare plans to 18 states withinside the US, gives cowl for dependancy remedy already below its fundamental healthcare plan.
However, there are specific plans which cowl specific portions and might produce other regulations associated with dependancy rehab remedy.
These plans additionally require specific premiums, in addition to deductibles. This approach that they provide specific insurance.
For example, their fundamental plan is usually less expensive however it would not cowl as tons as their trendy plan.
For this reason, it’s far critical to ensure which you have the best plan in your needs.
It’s critical to undergo in thoughts that Suboxone is commonly a part of a long-time period remedy plan and rehab program, so that you will want to test whether or not Suboxone is included through your coverage earlier than you begin your remedy.
Typically, Ambetter’s plans cover medicine or different pharmacy benefits. You might also discover that you ought to allow for a co-pay in case you need Ambetter to cover the costs of Suboxone.
If you’re uncertain whether or not you’re absolutely included in your Ambetter fitness plan, then it is excellent to talk to an Ambetter representative.
He may be capable of suggesting the precise charges and amount you’re included in with your policy.
Residential Treatment
One of the most intense forms of addiction treatment is residential treatment, also called inpatient treatment. This means that patients stay at a rehab center for a certain amount of time, and they receive therapy and medical care at the facility.
Ambetter Pharmacy Program Ambetter’s pharmacy program provides the appropriate, high quality, and cost effective drug therapy to all Ambetter members. Ambetter works with providers and pharmacists to ensure that medications used to treat a variety of conditions and diseases are covered.
Medication assisted treatment (MAT) is the use of medications, in combination with counseling and behavioral therapies, to provide a “whole-patient” approach to the treatment of substance use disorders.
Do All Rehab Centers Accept Ambetter Insurance?

Whether a rehab middle, medical institution or health practitioner permits coverage to cowl the patient’s fee is commonly as much as them.
Not all states in which Ambetter presents fitness care have alcohol or drug rehab centers which can be included with the aid of using Ambetter coverage.
However, your coverage might also cowl out-of-kingdom dependancy remedy. This manner that you’ll be capable of tour to your selected rehab middle to make sure you acquire the right remedy for you.
Depending to your plan and coverage, Ambetter can offer both partial or complete cowl for inpatient rehab centers that receive your coverage coverage beneathneath sure rules.
It can be difficult to find a doctor that accepts Ambetter insurance and also prescribes Suboxone. You may have to contact individual doctors in your area to inquire about their acceptance of Ambetter insurance and prescribing of Suboxone.
Some of Ambetter’s coverage plans additionally come up with the choice to search for dependancy remedy outdoor in their community providers.
Yes, many health insurance plans will cover rehab. Coverage varies depending on the type of plan and the specific treatment program. It is important to check with your insurance provider to find out what is covered and what is not.
However, this frequently comes with a better top rate or co-payment.
Does Ambetter offer Medicare and Medicaid?
If you have Medicaid coverage, you can apply for Medicare Advantage plans. Medicare provides coverage for people over 65. Medicaid provides financial assistance to individuals who have financial problems. Medicaid offers two kinds of coverages: mandatory and optional coverages. The government sets up the benefit which must be deemed necessary and your state determines whether the benefit must be optional. Medicaid may be required to provide substance abuse treatment depending upon your state.
Substance abuse services provide support to individuals struggling with substance use disorders. These services can include detoxification, inpatient and outpatient treatment, counseling and therapy, case management, relapse prevention, support groups and aftercare programs.
Mental Health Parity
The first effort happened in 2008 with the passing of the Mental Health Parity and Addiction Equity Act (MHPAEA) which mandates parity between mental health benefits and medical/surgical benefits. In 2010, the Affordable Care Act was passed that defined 10 essential health benefits that all marketplace health plans must cover.
Does Ambetter Cover Inpatient Addiction Treatment?
In recent years, addiction treatment has become an essential service for millions of Americans.
health plans meet this demand, many of which cover a wide range of medical needs.
One of the most intensive forms of addiction treatment is inpatient treatment, also called inpatient treatment. Completing inpatient treatment is an important milestone in the recovery process.
Addiction treatment services are professional programs designed to help individuals struggling with addiction. These services can include medical detoxification, inpatient and outpatient treatment, counseling, medication-assisted treatment (MAT), family therapy, and aftercare support.
Intensive outpatient programs (IOPs) are mental health treatment programs that provide a higher level of care than traditional outpatient services.
Staying in a rehabilitation center for a period of time to receive treatment and medical care.
The exact treatment and length of stay of a patient at the
The center will depend on the needs of the physician and the patient.
Amebetter typically covers inpatient rehabilitation programs. However, there are different levels depending on individual policies.
Not all rehab centers are covered by Ambetter, so it’s a good idea to check the policy before starting treatment.
How Long Does Ambetter Cover Suboxone Treatment?
Depending on your coverage plan and coverage, Ambetter might also additionally handiest cowl Suboxone remedy for a positive range of days.
As a rule of thumb, maximum healthcare insurers cover the fees of dependancy medicinal drug for as much as 30 days.
This is commonly the quantity of medicine for short-time period rehab. However, your coverage issuer can be capable of increase this period, as much as a most of 60 days.
Again, this does rely upon your coverage. If you aren’t completely covered, then it’s also profitable speakme to your selected rehab middle in which you’ll be capable of workout a price plan. Blue Shield of covers Suboxone as part of its prescription drug coverage.
Conclusion
Ambetter covers loads of dependancy treatments, which include medicinal drug together with Suboxone. The precise amount that Ambetter covers for Suboxone remedy relies upon for your coverage.
It’s fine to test your coverage cautiously earlier than you begin any dependancy remedy. If you can’t discover the precise info to your coverage, then it is a great concept to talk to a customer support guide at Ambetter.
- 20 Day Inpatient Alcohol Rehab - February 15, 2024
- Drug And Alcohol Rehab 77441 - February 15, 2024
- Alcohol Rehab York Pennsylvania - February 15, 2024